When Early Symptoms of Obesity Become a Medical Concern

What’s in This Article
This article focuses on how early symptoms of obesity that we usually ignore can progress into measurable medical concerns. It discusses why obesity is not just about weight gain, highlights the key medical indicators of obesity, and helps you understand when it’s time to seek professional care.
Early Symptoms of Obesity: Even Small Changes Matter
In our previous post on hidden signs of obesity, we looked at how obesity often begins with subtle shifts in our energy, sleep, and food intake. You might notice visible changes or persistent symptoms of obesity, like fatigue, excessive sweating, shortness of breath, etc. We may think of these early symptoms of obesity as small ripples in a pond, assuming they will eventually become manageable. However, there is often a specific moment, a ‘turning point’ if you will, when you realise these are no longer avoidable discomfort. They’ve become measurable medical concerns.
This is the stage where obesity stops being about how you look and starts being about how your body functions. Recognising this turning point can help you become more attuned with your body, approach a professional, and get the clinical clarity needed to reclaim your health. Today, we’re looking at the specific medical indicators for obesity that signal it’s time to go for professional care.
Weight Isn’t Just About Looks: Why Visual Judgment Can Fail
So, how do you know if you’re overweight or obese? Obesity isn’t always visible. Some people carry excess visceral fat, which is stored deep within the abdominal cavity or wrapped around vital organs like the liver, pancreas, and intestines. This internal fat isn’t always visible externally, meaning a person may look relatively slim, yet still be at risk. Weight-related issues often begin at the metabolic level long before fat becomes visible. This is why many people don’t realise they’re at risk until symptoms start interfering with daily
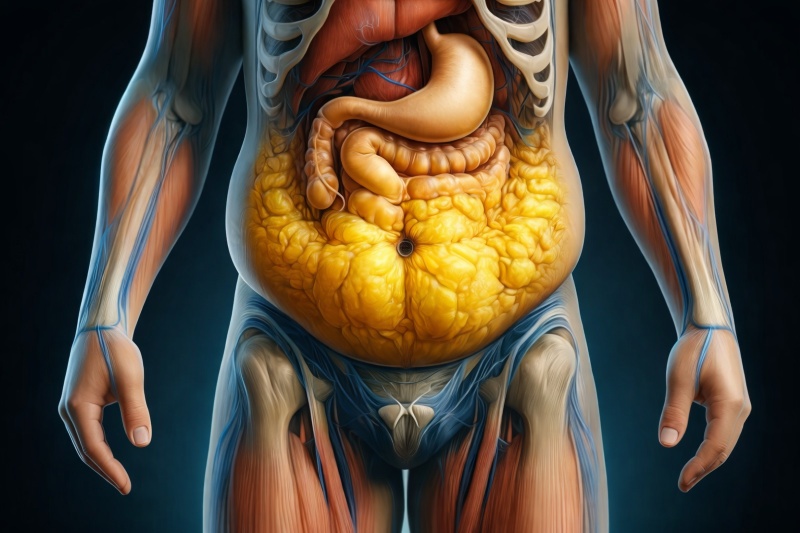
Medical Indicators That Suggest It’s No Longer “Just Weight”
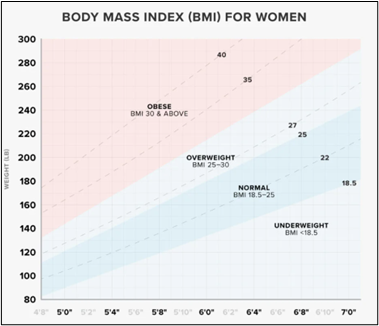
WHO defines overweight and obesity as abnormal or excessive fat accumulation that presents a health risk. Accordingly, a body mass index (BMI) ≥ 25 is considered overweight, and a BMI ≥ 30 is considered obese. However, BMI is not the only indicator of obesity. You can be ‘normal-weight’ on the scale and still be at risk for obesity-related complications. Here are some medical indicators that suggest you might be dealing with obesity:
- High Blood Pressure or High Cholesterol Levels: Excess body fat can disrupt normal cardiovascular functions, increasing strain on the heart and blood vessels.
- Rising Blood Sugar or Insulin Resistance: Early metabolic changes can reduce the body’s ability to use insulin effectively, even before obvious weight gain appears.
- Persistent Fatigue Despite Adequate Rest: Obesity can interfere with energy metabolism and sleep quality, leaving you tired despite sufficient rest.
- Irregular Menstrual Cycles: Hormonal imbalances related to excess fat tissue can affect ovulation and menstrual regularity.
- Frequent Heartburn or Digestive Discomfort: Increased abdominal pressure and slower digestion may trigger reflux and ongoing digestive symptoms.
These early symptoms of obesity may show up even before visible weight gain, easily missed unless you look for them, or if they’re revealed in your routine health check-up.
When Is the Right Time to See a Doctor?
We often ignore or avoid these early signs of obesity. However, if you’re noticing any of them persistently, procrastination will only increase your troubles. Reaching out to a doctor early on can prevent future issues and make weight management easier. Remember, it’s not just about losing weight, but also long-term health and well-being.
Awareness Is the First Step Toward Health
Obesity and weight gain creep in slowly with signs like fatigue, cravings, or sleep disturbances as their subtle indicators. We ignore these subtle signs, waiting for drastic weight changes to make things glaringly obvious. However, they are a signal of your body’s call for help. If you can recognise these signs at the initial stage and get help from the beginning, it becomes easier to improve your metabolism and energy levels, prevent future complications, and maintain a healthier weight.
Final Thoughts
The key point of discussing medical indicators is not just identifying what’s wrong with your body. It’s also about taking proactive steps to manage these early symptoms of obesity and reclaim your health. If you’re noticing any of these signs, it’s better to reach out to a professional and get the right guidance. A personalised health evaluation, with expert doctors at GP Northbourne, can make your wellness journey smoother, safer, and far more effective. You owe your body the care it deserves, and taking action today could be the step that makes all the difference.
Frequently Asked Questions
Yes. Obesity can exist internally in the form of visceral fat, which surrounds vital organs. A person may look normal or slim but still experience metabolic issues like insulin resistance, high cholesterol, or high blood pressure.
Common indicators include high blood pressure, abnormal cholesterol levels, rising blood sugar, persistent fatigue, digestive issues, and hormonal imbalances such as irregular menstrual cycles.
No. While BMI is a useful screening tool, it does not account for fat distribution or visceral fat. Someone can have a normal BMI and still be at risk for obesity-related complications.
EndomIf symptoms like fatigue, breathlessness, heartburn, or abnormal lab results persist despite lifestyle changes, it’s a good idea to consult a doctor. Early evaluation can prevent problems in the long term.etriosis itself does not directly cause weight gain. However, symptoms such as bloating, inflammation, hormonal changes, reduced activity due to pain, or side effects from treatment can lead to weight fluctuations. If weight changes occur alongside other symptoms of endometriosis, it’s worth discussing them with your GP.
Excess fat, especially visceral fat, interferes with insulin function and increases inflammation. This disrupts metabolism, leading to low energy levels, cravings, and difficulty managing weight.
Absolutely. Identifying obesity-related medical changes early makes treatment more effective, reduces the risk of chronic diseases, and supports sustainable improvements in health and energy levels.
Recent Posts:


Understanding Autism: Early Signs and Finding the Right Path Forward